What is a diabetic foot ulcer?
A diabetic ulcer is an open wound secondary to systemic changes due to longstanding effects of diabetes mellitus. These wounds are usually secondary to the effects of repetitive trauma on a nonsensate foot.
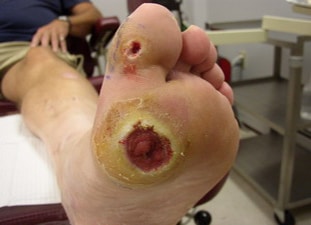
What are the effects of a foot ulcer?
Typically with longstanding diabetes, the patient will present with structural (both boney and muscular) changes in their feet and diminished sensation in their feet. With these changes, the patient will experience repetitive trauma to their feet (usually the plantar aspect of the forefoot) and not realize it.
How Common Are Foot Ulcers?
Diabetic foot ulcers occur in approximately 15% of patients with diabetes, and of these, up 24 % of ulcers will end in amputation. Amputations in patients with diabetes are associated with high morbidity and a 5-year survival rate of 31%.
Whos is at Risk for Developing a Diabetic Foot Ulcer?
Anyone living with diabetes is at risk of developing a diabetic foot ulcer. Of the more than 20 million people in the US with diabetes, as many as 25% will develop a foot ulcer in their lifetime. At particularly high risk, are those with either loss of sensation in their feet (neuropathy) or inadequate blood flow (ischemia). If you experience either of these symptoms, consult a doctor immediately.
Are Diabetic Foot Ulcers Painful?
A diabetic foot ulcer may not present in an expected manner. Relatively few patients experience foot ulcers as painful. The reason is neuropathy, a secondary symptom of diabetes in which the nerves in the extremities loose normal sensation. Some people do experience symptoms such as stabbing, shooting, or burning pain in the foot when a diabetic ulcer has formed.
What Are the Beginning Signs of a Diabetic Foot Ulcer?
If you are regularly examining your feet and extremities, you may quickly spot the early warning signs of a diabetic ulcer. You may see unusual redness, irritation or swelling in a foot. You may notice an unusual odor from one or both feet or stains on your socks that come from fluid drainage from the foot. If your diabetic foot ulcer worsens, your symptoms may include drainage or the darkening of tissue. This is a sign of inadequate blood flow to the tissue in the vicinity of the ulcer. If you notice any discoloration of foot tissue or other symptoms, contact our office in Glendale, AZ for appropriate treatment.
When Should I See a Specialist for a Diabetic Foot Ulcer?
Being a diabetic, you are more susceptible to nerve and blood vessel damage. This damage can result in reduced sensation, tingling, or numbness in your feet and extremities. As a result of the changes in nerve sensation, tissue damage may go unnoticed for some time. As a diabetic, it is imperative that you routinely observe the skin and tissue characteristics that appear over time. If any changes occur in the color or texture of your skin, you should schedule a consultation with your primary care doctor or with a vascular specialist. Your regular exams observe your skin and also evaluate your sensation and foot pulses to help determine the degree of neuropathy you may have.
What is the Most Effective Way to Treat a Diabetic Foot Ulcer?
Your primary care physician or vascular care specialist will help you determine the best method of managing your diabetic foot ulcer. Early, conservative treatment usually involves wound debridement. This minimally-invasive procedure involves the removal of diseased or infected tissue from the foot. Treatment also focuses on the prevention of infection expansion utilizing oral antibiotics or other therapies. Your doctor may advise you to cleanse your skin ulcer one or more times per day using approved cleansers and moisturizers. After cleaning, moisturizing, and treating your skin with a topical antibiotic, you may also need to cover the wound with a sterile bandage until your next cleaning. Severe diabetic foot ulcers may require the use of crutches or another assisted device that will keep the pressure off of the foot. Where there is less pressure, there is an ability to heal more quickly from tissue infection.
Does Getting My Blood Sugar Under Control Stop Recurring Ulcers?
It might. Studies indicate that dysregulated blood sugar levels are a strong contributor to tissue irregularities, including diabetic neuropathy and foot ulcers. The better you control your blood sugar, the more you reduce your chances of small sores or cuts becoming ulcerated. That said, even if you're checking your blood sugar regularly and seeing stable numbers, it is important that you closely examine the skin and sensation on your feet and lower extremities. You should also stay up-to-date with your routine medical examinations. Your doctor may catch new symptoms that you overlook. Signs that you should see your doctor include cracks, cuts, blisters, redness, thick calluses, white spots, or other changes in the tissue on your feet. Diabetic foot ulcers most commonly occur on the ball of the foot, often near the big toe. Observing these areas once every day, alongside routine blood sugar checks, can help you learn to manage your ongoing health utilizing diet, exercise, and other conservative remedies.
Why choose Dr. Zakhary for foot ulcer treatment
Dr. Zakhary has extensive experience and training in the treatment of diabetic foot ulcers. He is very passionate about wound care and limb salvage and understands the physical, social, and financial impact that such wounds can cause. If you or someone you know is living with a diabetic foot ulcer, please call our office today to schedule an appointment with Dr. Zakhary.
Schedule a Diabetic Foot Ulcer Consultation
If you're interested in learning more about diabetic foot ulcer treatment please contact us for a consultation at (623) 258-3255 or fill out our contact us form here. We will discuss your needs and concerns, and determine your best course of action.